There is a strong connection between mental health and equity, which has a significant and often negative impact on the people, communities, and health system of Ontario. These overlapping issues are wide-ranging, complex, and touch diverse regions and populations across the entire province. Consider that lesbian, gay, bisexual, trans, queer, intersex and Two-Spirit (LGBTQI2S) youth are over four times more likely to attempt suicide than their straight and/or cisgender peers. People with mental health and addictions issues also face discrimination on campus, in employment, in housing, and in many other essential and health-promoting areas of life. Furthermore, consider that Northern Ontarians face the highest rates of depression, hospitalization and medication use, but have access to less comprehensive, available and accessible mental health and addictions services and supports.1Canadian Mental Health Association Ontario. (2017). Advancing equity in mental health: An action framework. Retrieved from http://ontario.cmha.ca/wp-content/uploads/2016/07/PPE-0001-Advancing-Equity-in-Mental-Health-2.pdf
To help us better understand these issues, the Canadian Mental Health Association Ontario (2014)2Canadian Mental Health Association Ontario. (2014). Advancing equity in mental health: Understanding key concepts. Retrieved from http://ontario.cmha.ca/wp-content/files/2014/05/Advancing-Equity-In-Mental-Health-Final1.pdf has developed a framework called Advancing Equity in Ontario: Understanding Key Concepts. In this framework, they identify three dynamic and overlapping relationships between equity and mental health:
- Equity matters for mental health – Due to decreased access to the social determinants of health, inequities negatively impact the mental health of Ontarians. Marginalized groups are more likely to experience poor mental health and in some cases, mental health conditions. Marginalized groups also have decreased access to the social determinants of health that are essential to recovery and positive mental health.
- Mental health matters for equity – Poor mental health and mental health conditions have a negative impact on equity. And while mental health is a key resource for accessing the social determinants of health, historical and ongoing stigma has resulted in discrimination and social exclusion of people with lived experience of mental health and addictions issues.
- Equity and mental health intersect – People often experience both mental health issues and addictions and additional inequities (such as poverty, racialization, or homophobia) simultaneously. Intersectionality creates unique experiences of inequity and mental health that pose added challenges at the individual, community and health systems level. These issues disproportionately impact three clusters of populations: people with lived experiences of mental health and addictions issues; people who experience marginalization related to the social determinants of health such as sexual orientation, poverty, racialization and disability; and people with lived experiences who also experience additional marginalization related to the social determinants of health.

Defining Key Concepts: Equity
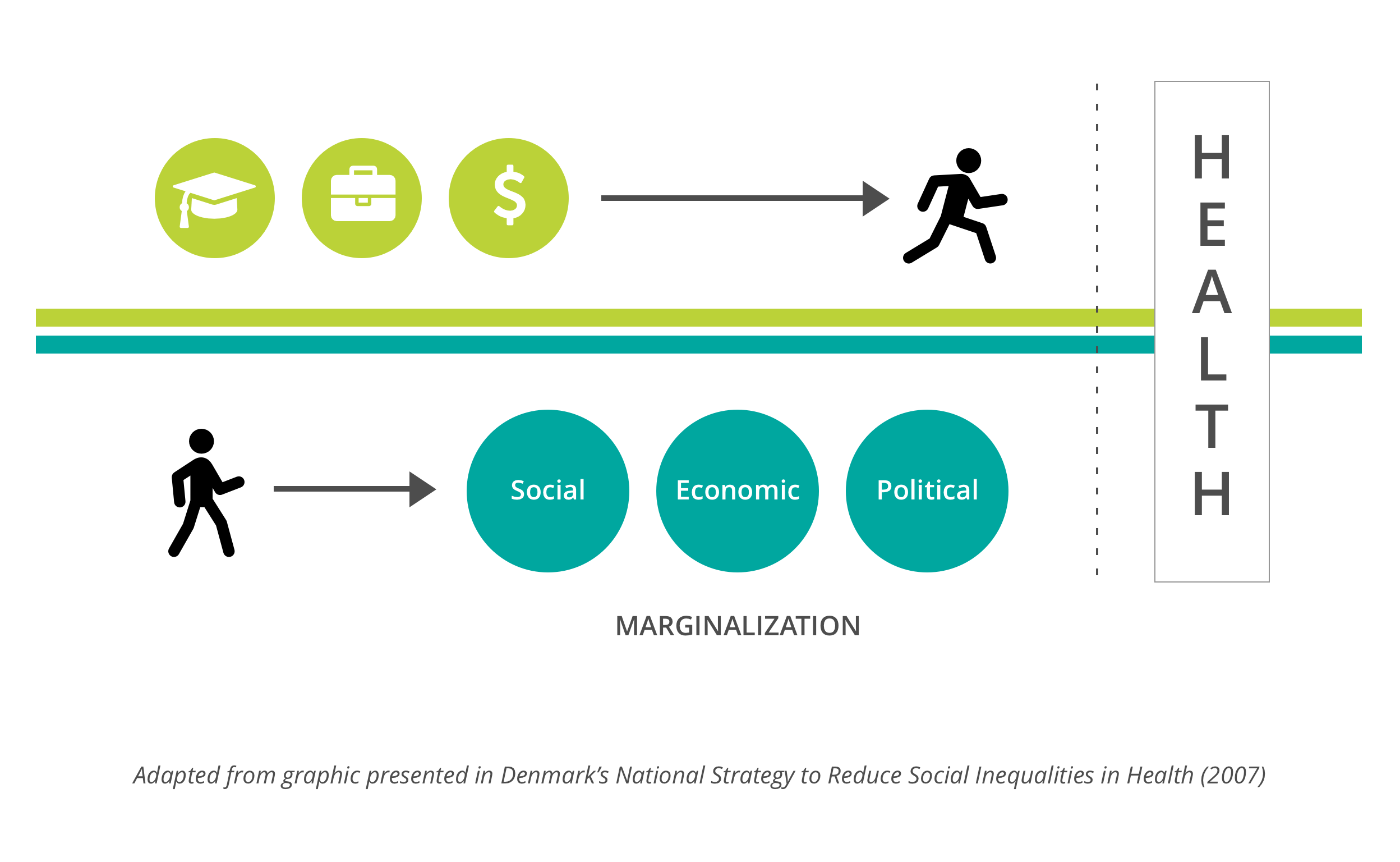
INEQUITIES can be understood as the social, economic and political marginalization (disadvantage or exclusion) that some groups face in society. EQUITY is a way to address marginalization. In contrast to equality, which seeks the same intervention for all individuals, an equity-based approach recognizes that different actions are required to achieve similar outcomes for different individuals or groups due to the uneven distribution of power, wealth and other resources in society. HEALTH INEQUITIES are systemic, avoidable and unfair differences in health outcomes, a sign of broader inequities in society.
From an equity perspective, marginalization is rooted in histories of differential access to power in society (such as racism, poverty and the stigma associated with mental health issues) and maintained by ongoing social, economic and political factors which can be called the SOCIAL DETERMINANTS OF HEALTH.
In Ontario, the social determinants of health include:
- Aboriginal status
- Disability
- Early life experiences
- Access to education
- Employment status and working conditions
- Food insecurity
- Access to health services
- Geography (rural/northern regions)
- Gender and gender identity
- Housing
- Immigration status or experience
- Income and income distribution
- Interaction with the justice system
- Race
- Sexual orientation
- Social exclusion, and
- Access to a social safety net
Three social determinants are particularly significant for mental health: freedom from discrimination and violence, social inclusion, and access to economic resources.
Experiences of marginalization INTERSECT. For example, a South Asian woman studying at a northern post-secondary institution may have just lost her part-time job, and also be living with bipolar disorder. Her life experiences are simultaneously informed by her gender, mental health, race, income and employment situation, and geography. Similarly, her lived experience of mental health issues and of the mental health system will be informed by all. It would be difficult or impossible to separate out the impacts of one factor from another. Instead, all factors must be considered together. Due to its deep and entrenched roots, addressing inequity requires complex systemic change at multiple levels and settings.
For more information, please read CMHA- Ontario’s discussion paper Advancing Equity in Mental Health in Ontario: Understanding Key Concepts (also available in French) and their new Equity Action Framework.
| ↑1 | Canadian Mental Health Association Ontario. (2017). Advancing equity in mental health: An action framework. Retrieved from http://ontario.cmha.ca/wp-content/uploads/2016/07/PPE-0001-Advancing-Equity-in-Mental-Health-2.pdf |
|---|---|
| ↑2 | Canadian Mental Health Association Ontario. (2014). Advancing equity in mental health: Understanding key concepts. Retrieved from http://ontario.cmha.ca/wp-content/files/2014/05/Advancing-Equity-In-Mental-Health-Final1.pdf |